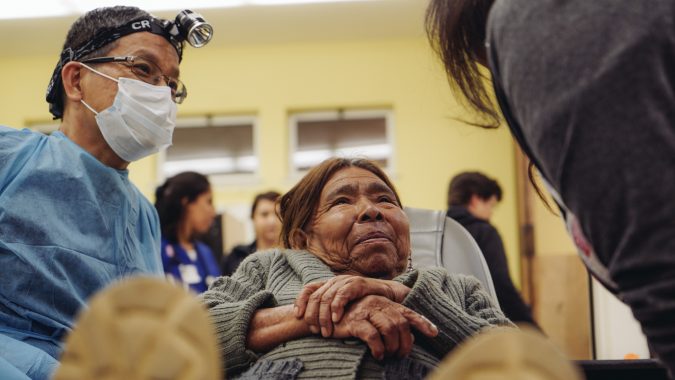
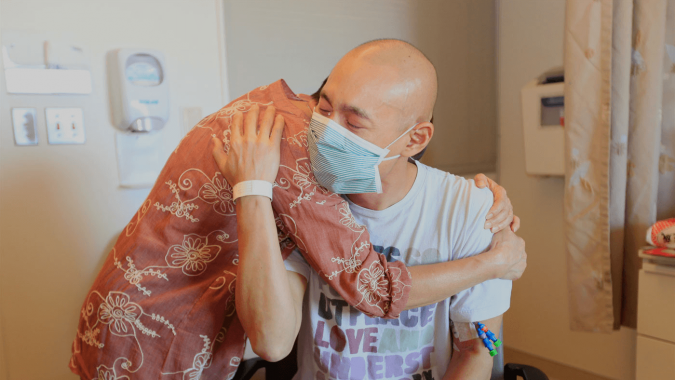
Nowadays, we have more ways to communicate and stay connected than ever before. But, has the quality of our relationships improved as a result? Some may argue yes, but former U.S. Surgeon General Dr. Vivek H. Murthy says not quite.
“During my years caring for patients, the most common pathology I saw was not heart disease or diabetes; it was loneliness,” he writes in the Harvard Business Review. He’s coined it as an ‘epidemic,’ suggesting loneliness is the underlying factor that gives way to the illnesses plaguing most Americans today.
How then, does it supposedly do so, what qualifies it as an epidemic, and what role can today’s medical professionals play in addressing this quiet threat to our health?
Let’s Talk About Loneliness
In his report, Dr. Murthy defines loneliness as “the subjective feeling of having inadequate social connections.” Whether we perceive our relationships as thin, superficial, or lacking in excitement or care, there is growing proof that our social lives impact our psychological health. Yet, how do we know it isn’t all just in our heads?
On the topic of his book on rootlessness in the United States, US Senator and author Ben Sasse indicates that factors as simple as property distance have reduced our interactions with neighbors and, therefore, meaningful connections. For example, 65 years ago, new homes were built out at 750 square feet, whereas today, the average size is 2,400. And this, he says, has impact.

In an interview with WNYC’s Brian Lehrer, Sasse mentions, “statistically, it’s less likely that you know the person who lives two doors down. And, yet, knowing the person two doors down is correlated with happiness- more social media friends [aren’t].”
Loneliness Strikes Back
Poring through countless studies, Dr. Murthy found “loneliness and weak social connections are associated with a reduction in lifespan similar to that caused by smoking fifteen cigarettes a day.” He also writes it causes a greater potential “risk of cardiovascular disease, dementia, depression, and anxiety.” How?
“Loneliness causes stress, and long-term or chronic stress leads to more frequent elevations of a key stress hormone, cortisol,” Dr. Murthy explains. And, the effects of cortisol and chronic stress are well-documented.
There’s no denying the digital revolution’s role in loneliness, too. “People sit in an office full of coworkers, even in open-plan workspaces, but everyone is staring at a computer,” points out Dr. Murthy. On a wider scale, it’s true; at work or home, we often communicate through sophisticated- and expensive- bits of hard plastic, glass, and metal.
So, we live in lonelier times. What’s the big deal?

According to the American Psychological Association, chronic stress can reverberate through our musculoskeletal, respiratory, cardiovascular, endocrine, gastrointestinal, nervous, and reproductive systems- to name a few- and can cause lasting damage.
Because of this rampant and widespread danger to our health, how can the medical community work to address loneliness head on?
The Humanistic Approach
Humanistic medicine, also referred to as patient-centered or values-based medicine, can be defined as the practice of compassion “to help our fellow humans and relieve suffering.” And, physicians who operate this way exhibit a key attitude and habit, according to Dr. Carol M. Chou.
In her survey of residents’ observations of physicians at the University of Pennsylvania, she discovered humanistic physicians approach “patients with a sense of humility and real curiosity about their lives, especially toward those patients to whom it may seem difficult to relate.” This outlook helps foster an earnest connection between patient and doctor.
And, if loneliness is about connecting, medical professionals are in prime positions to be ambassadors of warmth and welcome. Of course, there are challenges to this, acknowledges, Dr. Paul B. Rothman, Dean of the Medical Faculty and CEO of John Hopkins Medicine. They include time constraints, large volumes of patients and paperwork, and, of course, burnout.
Despite the obstacles, tackling loneliness head on will be vital for years to come. “Caring doctors are better doctors,” Dr. Rothman writes, “they practice safer medicine, earn more trust from patients and get them more engaged in their healthcare, leading to better outcomes.”

Healing One Another, One Connection at a Time
While a trip to the doctor’s office is by no means a magic pill, it’s an excellent place for patients and health professionals to have intimate, trusted, and meaningful connections. For the rest of us, it’ll be our mission to cultivate strong and genuine social bonds with others, and to then reap the rewards that come from feeling like we’re not so alone after all.
Discover all about our approach to humanistic medicine and register for the 2019 TIMA Global Forum.